A new clinical trial offers hope
Eventually, she was contacted by HonorHealth Research Institute’s GI/Bariatric Research Division about a new, less-invasive clinical trial involving a device called the Omega-Cuff. Shaped like the Greek letter Ω, the cuff is designed to prevent excessive acid from entering the esophagus while allowing much of the normal swallowing process to remain intact.
The device, part of a first-in-human study, is placed on top of the esophageal sphincter muscle, just above the stomach. In laboratory studies, the device increased resistance to acid reflux, but did not interfere with normal food swallowing. This is a permanent implant, and that is just fine with Debra.
“Since that surgery, I have not had to take any acid-reflux medicine,” shares Debra, who feels “wonderful” and is grateful for the simple act of bending over, “without puking.”
She visits the Research Institute for monthly follow-ups, describing her care as “very awesome.” She describes the device as “the best thing ever!”
“I am so excited – there’s no negative impact,” Debra explains. “And I can eat spicy food! It’s wonderful.”
Related content
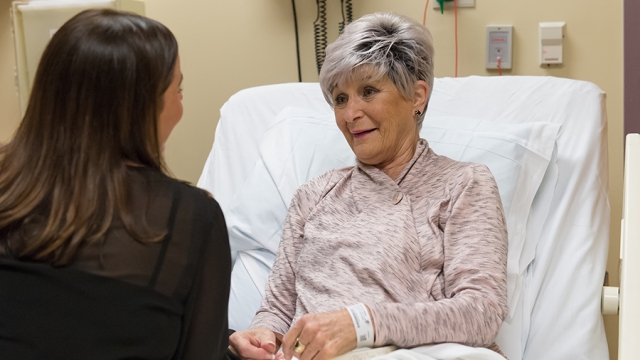
Offering patients innovative treatment options
The HonorHealth Research Institute is at the front of today’s most important health questions. Established in 2005, the Institute has become a patient destination for treatments often available nowhere else.
GERD: heartburn treatment options
If you’re reaching for antacids regularly to combat heartburn, you may suffer from gastroesophageal reflux disease, commonly known as GERD. Check out tips to reduce heartburn and when to see a doctor.

COPD patient breathes easier after clinical trial
Lourdes, who suffered for more than 12 years with COPD, enrolled in a clinical trial with a non-surgical procedure called targeted lung denervation. It is designed to reduce airway nerve activity linked to COPD flare-ups.
